The Lowdown on the COVID-19 vaccine, periods and fertility: Your questions answered
What's the lowdown?
There’s no evidence that getting the COVID-19 vaccine impacts male or female fertility or the ability to conceive
Any changes to your menstrual cycle after the vaccine are temporary
It is common for other external factors such as weight, exercise and stress to temporarily impact the menstrual cycle
Any menstrual changes caused by the vaccine or other factors does not mean that your fertility is impacted in the long term
In partnership with the NHS, The Lowdown sits down with Dr Viki Male and Dr Fatima Husain to discuss the latest research on the COVID-19 vaccine, fertility and periods
What’s the lowdown on catching COVID-19?
- There is evidence that catching COVID-19 can temporarily impact male fertility by reducing sperm count and quality
- There is also evidence that catching COVID-19 during pregnancy can have detrimental effects for both you and your baby towards the end of pregnancy and after birth
In partnership with the NHS, we ran a survey to gather information on the main concerns of young women and people who menstruate on the COVID-19 vaccine and its effects on periods and fertility, which showed that changes to menstrual cycles were a concern. In this guide we cover the latest evidence around the vaccine, alongside other external factors that can affect the menstrual cycle. You can also watch the webinar for more insight from Dr Viki and Dr Fatima.
Does the vaccine impact pregnancy in clinical trials?
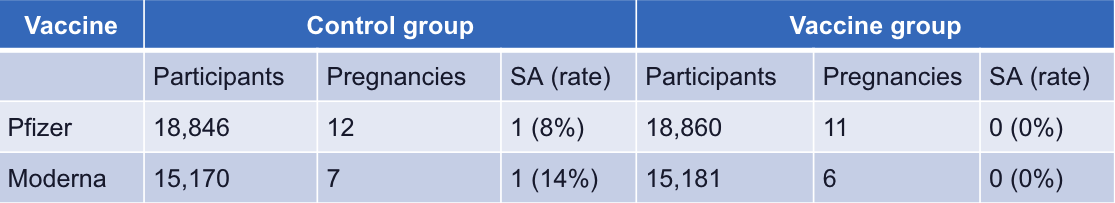
In these clinical trials for Pfizer and Moderna, participants were asked to use reliable contraception. There were some accidental pregnancies (this is to be expected, as no method of contraception is 100% effective), but these happened at basically the same rate, despite whether a participant had received the vaccine or the control.
This shows that the vaccines in these trials did not reduce the chances of participants becoming pregnant – both pregnancy rates are low because every one of them was on contraception. Furthermore, the miscarriage rate (SA rate) was also more or less the same across the vaccinated and non-vaccinated groups.
Will getting the COVID-19 vaccine affect my fertility?
No, there is no evidence that having the COVID-19 vaccine impacts either male or female fertility. There have been a range of studies in this area, with the first evidence coming from IVF clinics (see references). Across these studies, it has been shown that in IVF settings there’s no difference in clinical pregnancy rates and in other measures of fertility – such as ovarian function, egg quality, and fertilisation – between vaccinated and unvaccinated patients. Three of these studies specifically looked at fertility rates before and after vaccination, too. But does this still apply if you’re trying to conceive naturally? In short, yes.
A 2022 US study tracking more than 2000 couples trying to conceive ‘spontaneously’ over the course of 10 months also found that COVID-19 vaccination makes no difference to both male and female fertility on your chance of conception, and in the months that you have the vaccine there’s not even a temporary difference.
Multiple studies have shown that COVID-19 vaccination does not alter sperm count or quality, or reduce the chances of conception for a male partner (see references).
The really interesting thing this study found was that while catching COVID-19 doesn’t affect female fertility, it can affect male fertility. It found that if a male partner had COVID-19, a couple would be less likely to conceive for two months after this, as COVID-19 infection reduces sperm count and quality for around 60 days.
Will the vaccine affect my periods?
There’s been lots of anecdotal evidence of people reporting either heavier, later, shorter and lighter periods, and there weren’t any significant studies around this for what felt like ages. Due to the fact that there are many external factors that can affect periods (we’ll come to that in a moment) which causes a natural variation in cycles anyway, it was difficult to know whether the changes that people were noticing were down to the vaccine, or because they were paying more attention to their cycles after the vaccine as they were expecting a change.
There are now two large, well-designed studies which looked specifically at these changes. One by the digital contraception app Natural Cycles, and another from Norway. The Natural Cycles study looked at period delays. It compared 2403 participants who had the vaccine with 1556 participants who didn’t. They found that the first dose of the vaccine in this cohort didn’t cause any delays to periods. The second dose of the vaccine, however, delayed the next period by only half a day.
The main change noted in this study was found in participants who had both of their vaccines in the same cycle, which resulted in a 2.3 day delay to their next period. Despite this delay, these participants’ cycles were back to normal two months after. (Note that in the UK, it is unlikely that you will have two doses of the vaccine within the same menstrual cycle). In short, any changes to your menstrual cycle after COVID-19 vaccination are small and reversible.
In the Norwegian study of 6000 participants who had regular periods, 37.8% of unvaccinated people reported a change to their period. This creeps up to 39.4% noticing a change after the first dose of the vaccine, and 40.9% after the second dose. The main change being that they experienced a heavier period. At the point of publishing, they hadn’t tracked it long enough to see when this effect was reversed. However, it shows that the differences are still small. In terms of periods being delayed, this study couldn’t find any delay when they asked participants to reflect on their previous periods – so while we can see these small changes in analysed data (the Natural Cycles study), anecdotally many of us may not notice a delay.
Does this evidence also apply to the booster vaccine?
None of the above studies specifically look at the booster vaccine, but it is highly likely that the evidence shown for the first and second doses will also apply to the booster. This could be a small delay to your cycle, or a potentially slightly heavier period than normal. Or, you may not experience any changes at all!
Why might the vaccine have an effect on my periods?
There’s no strong evidence as to exactly why, but Reproductive Immunologist, Dr Viki Male, suggested two possibilities for this in our webinar. Firstly, the immune system and sex hormones can cross-talk. So if the immune system has a big stimulation, i.e. the vaccine, that could potentially have a temporary effect on sex hormones. The sex hormones drive periods, so this could potentially cause a delay, or make them heavier. Secondly, the lining of the uterus is rich in immune cells which are important for the build up and break down of the uterus lining as part of the menstrual cycle. If we have this big immune stimulation, this could also potentially affect those cells and how they build up or break down the uterus lining.
What else can cause changes and irregularities to periods?
As we’ve established, there’s a lot of cross-talk that happens between your brain and your ovaries, which means that there are numerous things that can impact your period flow, cycle length, and even stop periods altogether, including:
- Too much exercise or stress
- Being overweight (generally BMI over 30) or extreme changes in weight
- Puberty and menopause (if periods suddenly become irregular before the age of 45 this needs investigating)
- Medical conditions such as polycystic ovary syndrome (PCOS)
Changes to your cycle because of the factors above would last longer than two to three cycles. They should not be attributed to the vaccine side-effects and if symptoms persist these should be investigated, so please see your GP.
It’s important to remember all forms of hormonal contraception and some non-hormonal such as the copper coil (IUD) can impact your periods. Take a look at our contraception pages and reviews to see what other users of each method have experienced, or take our contraception quiz to see which form of contraception is recommended best for you. Pregnancy is also a reason for periods to change and stop altogether so consider doing a pregnancy test as no contraceptive method is 100% effective.
When should I be worried about irregular periods?
How can you tell if it’s a side effect of the vaccine, or if it’s something else?
Vaginal bleeding can have many causes including polyps, infections, or cervical ectropion. If you’re still experiencing unusual bleeding after two cycles, then it’s not down to the COVID-19 vaccine. The MHRA advises: “anyone experiencing changes to their periods that are unusual for them, persist over time, or has any new vaginal bleeding after the menopause, following COVID-19 vaccination, should contact their doctor.”
Here’s what you should look out for:
- Constant bleeding, or bleeding for longer than 7 days each cycle
- Bleeding between periods
- Bleeding after sex regularly
- Cycles longer than 6 weeks, continuing for several cycles
- STI symptoms
When it comes to bleeding between periods, bleeding and spotting at the time of ovulation can be normal for some. However, if you’ve noticed bleeding that becomes heavier, or lasts a few days between periods, then it’s best to get it checked out. It’s also important to make sure your cervical smear tests are up to date!
If I don’t get the vaccine and I catch COVID-19, will that impact my periods?
Like a lot of illnesses, there’s evidence to show that if you get COVID-19, it can temporarily affect your menstrual cycle. One study looked at how COVID-19 infection might impact the menstrual cycle, specifically analysing sex hormones. While it couldn’t find a particular difference to hormones it did find that a quarter of participants reported changes to their period after catching COVID-19. Another study looking into the effects of long COVID also found that 15% reported changes to their periods after infection.
Dr Viki shares this advice: “if you’re really worried about your periods, not getting vaccinated is not the solution”.
Is it safe to get the vaccine if you’re pregnant?
Yes, it is safe to get the COVID-19 vaccine if you’re pregnant. There are now multiple studies across more than 185,000 people who have been vaccinated whilst pregnant, looking for things like increased risk of miscarriage, premature birth, stillbirth, the baby being born smaller than expected, and congenital abnormalities. No increased risk for any of these has been found from COVID-19 vaccination. Links to these studies can be found below.
There is strong evidence that COVID-19 infection in pregnancy can have a detrimental impact on you and your baby, however, particularly during the second term of pregnancy. There is an increased risk of premature birth, pre-eclampsia, stillbirth or infant death shortly after birth. This is why, like the flu and whooping cough vaccines, the NHS offers the COVID-19 vaccine to everyone who is pregnant. If you’re planning on getting pregnant, or are pregnant, and are currently unvaccinated, it’s important to consider these risks and COVID-19 vaccination will give you the best chance of avoiding them.
What about vaccinating young girls who have just started menstruating, or who haven’t yet begun?
Less research has been done on younger people, partially because it’s been the 18+ age group who have been vaccinated. It’s also harder to do research on children and this type of research is tougher because the menstrual cycle varies so much when you just start having periods. It can take up to eight years for your brain and ovary connection to mature, so it’s really hard to know what the normal is for somebody aged 11. If you notice a change in your child, or they notice a change, that could just be normal pre-teen and teenage period cycles taking a while to settle down.
How does the COVID-19 vaccine work?
The effects of vaccines come in two waves. The first is the innate immune response which happens straight away, causing sore arms, fever and headaches etc. This could potentially be the cause of the small, temporary changes to periods too. The second wave is the adaptive immune response which kicks in after around 10 days, and lasts for about 28 days. This is what gives you protection against COVID-19 infection. In some cases, this response can also cause side effects, which will appear within 28 days. Studies usually track any effects up to 6 months, anything that hasn’t appeared within that time isn’t likely to happen after, because the vaccine is actually only active in your body for 7 days, with the immune response then being active for 28 days.
For ongoing information on the latest evidence around the COVID-19 vaccine, menstrual cycle and fertility, check out Dr Viki’s handy online explainer document.
IVF setting studies:
- https://journals.lww.com/greenjournal/Fulltext/9900/In_Vitro_Fertilization_and_Early_Pregnancy.378.aspx
- https://academic.oup.com/humrep/article/36/9/2506/6345462
- https://www.medrxiv.org/content/10.1101/2021.05.30.21258079v1.full.pdf
- https://www.sciencedirect.com/science/article/pii/S2666334121000684
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8116639/
Effects on male fertility after vaccination studies:
- https://jamanetwork.com/journals/jama/fullarticle/2781360
- https://www.medrxiv.org/content/10.1101/2021.04.30.21255690v1.full.pdf
Getting the vaccine during pregnancy studies:
- https://www.nejm.org/doi/full/10.1056/NEJMoa2104983?query=featured_home
- https://www.nejm.org/doi/full/10.1056/NEJMc2113891
- https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-09-22/09-COVID-Olson-508.pdf
- https://jamanetwork.com/journals/jama/fullarticle/2790607
- https://www.nature.com/articles/s41591-021-01666-2
- https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-09-22/10-COVID-Kharbanda-508.pdf
- https://jamanetwork.com/journals/jama/fullarticle/2784193
- https://www.nejm.org/doi/full/10.1056/NEJMc2114466
- https://jamanetwork.com/journals/jama/fullarticle/2782047
- https://www.ajog.org/article/S0002-9378(21)00873-5/pdf
- https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1050721/Vaccine-surveillance-report-week-4.pdf
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8378017/
- https://www.sciencedirect.com/science/article/pii/S0264410X21011919?via%3Dihub
- https://www.cdc.gov/mmwr/volumes/71/wr/mm7101e1.htm
- https://jamanetwork.com/journals/jamapediatrics/fullarticle/2788938
Our medical review process
This article has been medically reviewed for factual and up to date information by a Lowdown doctor.