Cervical ectropion (erosion): symptoms, causes & treatment
In this article
What's the lowdown?
A cervical ectropion is where the soft cells from the inside of the cervix move to the outside
It is very common and if left alone will disappear as you get older
Cervical ectropion symptoms include increased discharge as well as pain or bleeding during or after sex
The combined pill contains estrogen which can increase cervical ectropion therefore you may wish to switch to a non-hormonal or progesteron-only contraceptive method to reduce symptoms
Cervical erosions do not increase your risk of cervical cancer
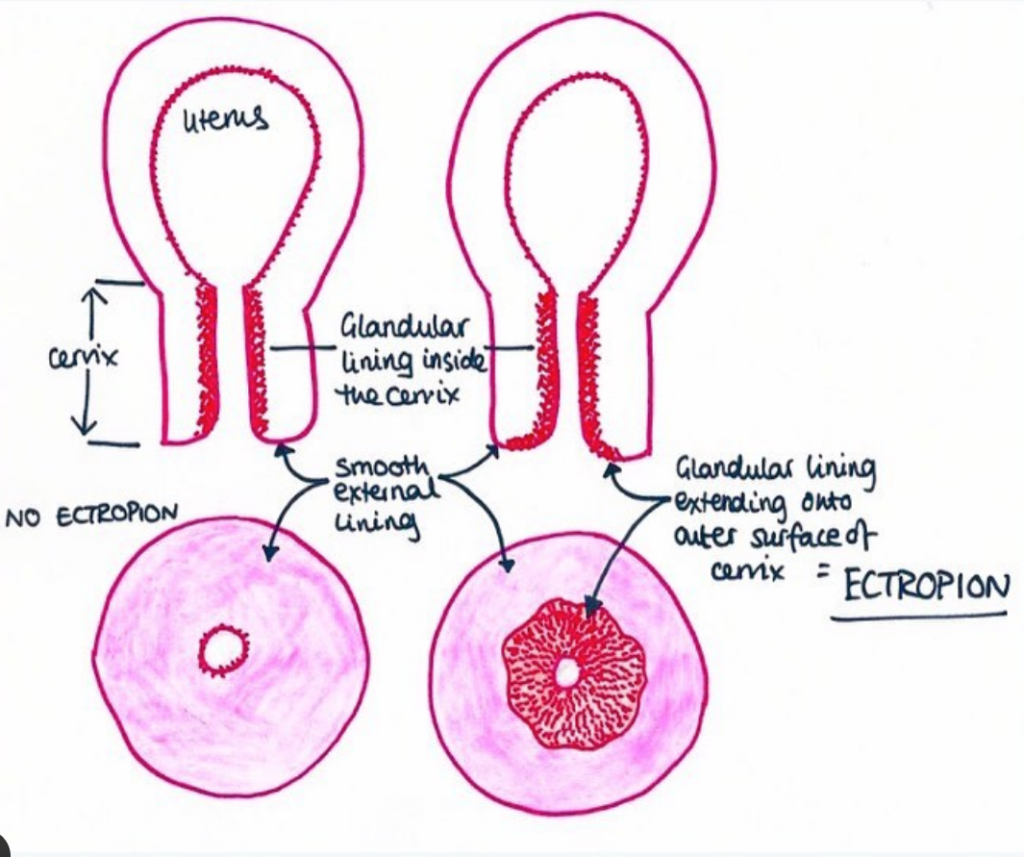
Big thank you to @gynaegeek for letting us use her brilliant cervical ectropion diagram!
My experience of cervical ectropion
Have you ever been for a routine smear or gynae examination, and having gone through the drama of getting half naked and deep breathing through the embarrassment, been told that you have a “cervical ectropion”?
Did those unknown words send shivers of anxiety through your body? Well, it did for me as a young medical student and hopefully, this will help calm some of your nerves.
It was after I had my first Mirena IUS coil fitted. I had found the procedure OK and after the first 2 months or so of slight anxiety and jawline acne, I was absolutely loving the endless possibilities of a period free life. I felt more comfortable and confident around sex until one drunken Saturday night after the deed, it looked as though a small animal had been sacrified on my sheets. There was blood everywhere.
Having learnt from lectures that bleeding = bad. I quickly took myself off to the GP. She promptly told me to wee on a stick before asking me to assume the position for a speculum examination and swabs. Thankfully, pregnancy was excluded which gave me a moment to allow the sweat to cool on my palms before she joyfully announced that I had a cervical ectropion. This was “a benign finding and nothing to worry about” so I was sent on my way.
At this point, I hadn’t reached the gynaecology phase of my university lectures so turned to Wikipedia and found very little information. So now, as a Medical Director of The Lowdown, here is what I wish I’d known then…
What is a cervical ectropion?
A cervical ectropion (sometimes called a cervical erosion) is a normal finding in young women of reproductive age. It is common and prevalent in between 17-50% of people with wombs including up to 80% of sexually active adolescents. They often cause no problems at all and can be found on routine smears.
To understand what an ectropion is, we need to talk about anatomy and pathology. The cervix is a tube-like structure at the top of the vagina connected to the uterus – we often refer to it as “the neck of the womb”.
The inside of the cervix is lined with a certain type of cell. This cell type is glandular which means it is soft, produces lots of mucus and bleeds more easily if it is hit by something (e.g. a penis). On the outside of the cervix, which your doctor can see during a smear test, the cells are harder, produce less mucus and are less likely to bleed.
In a cervical ectropion, the soft, red, mucous producing cells from the inside of the cervix, move onto the outside of the cervix. Here, you can see a redder, well defined ring around the cervix opening which is how healthcare professionals make the diagnosis.
Cervical ectropion symptoms
Now we understand what a cervical ectropion is, the symptoms may not surprise you. Women may suffer from increased vaginal discharge (the most common symptom), bleeding after sex (in 5-25% of women with an ectropion), pain after sex or occasionally bleeding in between periods.
Please ALWAYS see you GP if you notice a change in your discharge, bleeding after sex or bleeding in between periods to confirm if a cervical ectropion is the cause.
Cervical ectropion causes
Cervical ectropion is caused by hormonal changes. This is why they are more common in younger people, people going through puberty, pregnant women and those using certain contraceptives.
How is a cervical ectropion or erosion related to contraception?
The changes in the cells lining the cervix are driven by oestrogen and a change in the oestrogen/progesterone ratio in your body. Pregnancy and combined hormonal contraception can therefore increase the chance of a cervical ectropion.
We know that a number of our Lowdown community who have used our Get Advice service have suffered from symptoms related to cervical ectropion. These symptoms may affect your contraceptive choice and you may want to stop taking the combined pill.
Cervical ectropion and pregnancy
Having a cervical erosion does not affect your fertility, so you are just as likely to fall pregnant if you are trying to conceive. Once you are pregnant, the higher levels of oestrogen circulating in your body can cause cervical erosion so they are commonly seen in pregnant women. Remember, if you do have any bleeding in pregnancy, be sure to see a doctor for examination, even if you are known to have a cervical ectropion.
Cervical Ectropion / Erosion v Cancer
You may worry, but please don’t, there is no evidence that a cervical ectropion increases the risk of getting cervical cancer. Cervical ectropion and cervical cancer are completely separate conditions, with different causes and are not linked at all.
Cervical ectropion treatment
- Diathermy. This treatment uses an electrical current running through a small metal instrument to remove the ectropion cells on the cervix. It is usually carried out with local anaesthetic to numb the area.
- Cryotherapy. A small thin instrument with liquid nitrogen on the tip is used to freeze away the cervical ectropion cells. This can be done without local anaesthetic and should not be painful. Some women describe some mild cramping pain and feeling warm throughout their body.
- Silver Nitrate. This is another substance which can be placed on a small thin stick and pressed against the cervical ectropion to remove the cells. It should not be painful but can feel either warm or cold.
What happens during treatment for cervical ectropion?
You will be asked to lie on a bed and a speculum will be inserted to look at the cervix. This step is very similar to a cervical screening smear test.
If local anaesthetic is needed, this may sting as it starts to work. Any of the treatments above should not take any longer than 10 minutes.
If you are uncomfortable at any point, let a healthcare professional know.
What happens after treatment?
You can leave the clinic 15 minutes after treatment, and you are able to drive if you would like to. For 2 days afterwards, you may experience period like cramping, light bleeding or watery discharge. If this continues or gets worse, or you develop a fever then see a doctor.
You should avoid using a tampon or penetrative sex for 4 weeks after treatment.
Occasionally, a cervical ectropion may return. You are able to have another treatment but it is recommended to wait for at least 6 weeks between treatments.
Other things I wish I’d known…
- If left alone, cervical ectropions will disappear as you get older.
- Cervical ectropion does not increase your risk of cervical cancer. At all.
- Cervical ectropion might make you more susceptible to STIs including chlamydia. This is because the bug which causes chlamydia likes to infect the softer, glandular cells found within an ectropion. Some studies have found an increased risk of gonorrhoea and HIV infection, although this is still being debated within the research world. So, as always, you may consider getting regular STI checks and using condoms with new partners.
Our medical review process
This article has been medically reviewed for factual and up to date information by a Lowdown doctor.