Does alcohol affect the pill?
In this article
What's the lowdown?
Alcohol has no direct impact on the efficacy of the contraceptive pill (how well it works to prevent pregnancy)
Long term over use of alcohol and very heavy drinking can affect the liver and how it breask down the pill, making it less effective
Drinking can lower inhibitions and may lead to sexually risky behaviour, or forgetting to take your pill
For those taking oral contraceptives, vomiting whilst hungover may class as a missed pill – see our missed pill calculator to help you figure out your next step
The copper coil as emergency contraception is not affected by alcohol
Levonelle and ellaOne (the morning after pills) are not affected by alcohol – unless you vomit, in which case you may want to consider the copper coil
From a few drinks with friends at your local, to a cosy night in with your partner with a bottle of red, socialising with your loved ones can often involve a little social lubricant: alcohol. And it can be all too easy to throw caution to the wind and drink a *little* more than your next-day-hungover-self will thank you for! But if you’re taking the contraceptive pill, you may not have considered the impact of alcohol on its efficacy. Here’s what you should know.
NHS advice suggests men and women should not regularly consume more than 14 units of alcohol in a week, spread out evenly over three or more days. But how many of us know how to count our units?
If you’re drinking spirits, it’s pretty straightforward to keep track of your alcohol consumption; a single shot (25ml, ABV 40%) is one unit, a double is two. Easy! But beer and wine are a little harder to judge, particularly with the variation in strengths. For example, a small glass of wine ABV 12% is 1.5 units, compared to the same size glass of wine at 14%, which is 1.75 units. Did anybody bring a calculator?
Thankfully, the NHS has a handy guide to calculating the units in a drink. Alternatively, Alcohol Change has an online unit calculator that does all the calculations for you!
How does alcohol affect the birth control pill?
Enzymes (proteins in the body which help the breakdown of chemicals and drugs) in the liver are required to process the progestogen and oestrogen hormones in both the combined and progestogen-only pills.
Long term excess alcohol use can make these enzymes work faster, meaning the pill is broken down more quickly and can become less effective at preventing pregnancy.
Some medications (called enzyme-inducing drugs) can have the same effect and reduce the effectiveness of contraceptive pills. Drugs used in the treatment of epilepsy, as well as some antibiotics like rifampicin and the herbal remedy St John’s Wort, can all reduce the effectiveness of birth contorl pills.
Consuming alcohol socially and within safe limits does not directly affect how the pill works. However, severe alcohol abuse over a long period of time may cause scarring of the liver, known as cirrhosis. This can lead to liver failure and be life threatening.
Unfortunately, women suffering from severe cirrhosis of the liver also have a limited choice when it comes to contraception. They are unable to break down hormonal contraceptives, which results in ineffective contraception. Copper coils which don’t contain hormones can be a great alternative for women with cirrhosis.
On a serious note
Long term effects of alcohol misuse include an increased risk of:
- liver disease
- liver cancer
- breast cancer
- bowel cancer
- heart disease
- stroke
It’s perfectly normal to want to celebrate with a glass of wine in hand, but if you are concerned about the amount you’re drinking, reach out to your doctor. You may find yourself regularly drinking more than the recommended 14 units a week or reaching for a drink first thing in the morning. Friends may be voicing their concerns, or you may yourself feel guilty about the volume of alcohol you are consuming. These are all signs you could be misusing alcohol, so don’t be afraid to ask for help.
So, now we’ve looked at the science behind alcohol, it’s worth thinking about the ways drinking can indirectly impact the efficacy of contraception as a whole.
When the missed pill ‘hangxiety’ strikes
As you wake, bleary-eyed and a little worse for wear, reaching for your pill may not be at the forefront of your mind. So when the hangover has worn off, the sudden realisation of the time, and the unmistakable fact that you’ve missed your pill by more than a good few hours, can hit you like a hangover all over again. Alternatively, you may have missed taking your pill the previous evening whilst you were enjoying drinks with friends.
Missing a pill may have implications for its efficacy, so it’s important you know what to do. At The Lowdown, we’ve got you covered. Our missed pill calculator is designed to replace the confusion of patient information leaflets and the sense of unease with a series of simple questions designed to set out your next move. Our doctors have done all the hard work for you, and it may not be the case that one missed pill equates to a sudden dash to the pharmacy (although be prepared, it might!).
The progestogen-only pill is a bit of a slave to routine, and for the traditional progestogen-only pills like Noriday or Norgeston, a pill missed by as little as 3 hours can result in loss of protection against pregnancy.
Progestogen only pills containing desogestrel have a longer 12 hour window. Take the missed pill as soon as you remember and use extra contraception for the next 48 hours.
Check out our diagrams on pill ‘safe windows’, to help you determine whether you’re still in the time frame of being able to take your type of pill without it counting as being missed…



If you have remembered to take your pill, vomiting whilst hungover may have an impact on the absorption of your contraceptive and therefore its effectiveness. If this happens within 3 hours for those taking the combined pill, or within 2 hours for those taking the progestogen-only pill, take another pill right away and the next pill at the usual time. If you continue to vomit, however, you will need to think of this as a missed pill.
Consult our missed pill calculator for more info regarding the need for emergency contraception. If you’re in any doubt, seek the advice of a medical professional.
The morning after pill
Lowered inhibitions as a result of alcohol may lead to more than a cheeky snog, and if contraceptives weren’t used in the way they should have been – think: badly put on condoms or forgotten diaphragms – knowing your options for how to deal with these scenarios is what The Lowdown is all about.
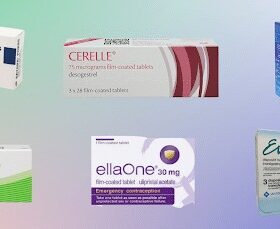
If you’re concerned about the possible lack of contraception you used the night before, emergency contraception is your friend. The morning after pill – either generic levonorgestrel-based pills like Levonelle or ellaOne – or the IUD, known more commonly as the copper coil, are the two options available.
Levonelle should be taken within 3 days of unprotected sex, whilst ellaOne gives you a little more time, and may be taken up to 5 days after unprotected sex. However, both morning after pills have a greater efficacy the sooner they are taken.
Does alcohol affect the morning after pill?
The morning after pills are not directly affected by alcohol. However there are a few important factors to remember when it comes to the morning after pill.
One: the morning after pill is thought to work by preventing or delaying ovulation (when an egg is released). If you are at a point in your cycle when you have already ovulated but you are at risk of pregnancy (this will be around day 14 in a typical 28-day cycle. although it varies from person to person), then the morning after pill will be ineffective.
Two: if you are sick within 2 hours of taking Levonelle or 3 hours of taking ellaOne, you’ll need another dose for it to work effectively. Alternatively, you may want to consider an IUD.
But don’t panic. The copper coil is a much more forgiving option and doesn’t care about vomiting or whether or not you’ve ovulated! It can be fitted up to 5 days after unprotected sex or up to 5 days after your earliest possible ovulation date, and is the most effective form of emergency contraception – less than 1% of women become pregnant when using the copper coil.
So you may wish to consider this even if the morning after pill is a viable option. What’s more, the copper coil can remain in place for around 5 to 10 years, depending on the brand of IUD, and will continue to act as a contraceptive during this time.
Let’s talk about STIs
Now we’ve got the pregnancy scare out the way, it’s time to look at the other consequences of a contraceptive-free hook-up. Condoms provide an excellent barrier to STIs and if you find yourself worried about the potential fallout from not using them, get yourself checked. Unprotected sex, particularly with a new partner, puts you at risk of chlamydia, gonorrhoea and a whole host of other sexually transmitted delights. Read our guide to get the lowdown on all things STIs.
If you’re struggling with missed pills or you just feel unsatisfied with your current method of contraception, you can book an appointment with one of our amazing doctors at The Lowdown. They can talk you through all your contraceptive options and find the perfect match for you and your lifestyle. Alternatively, you can compare side effects, effectiveness and risks of all the contraceptives featured on our website with our comparison tool.
Our medical review process
This article has been medically reviewed for factual and up to date information by a Lowdown doctor.