The Hormonal Coil – all your questions answered
The Hormonal coil (aka the hormonal intrauterine device, intrauterine system or IUS) is women’s favourite method of contraception here at The Lowdown. The Hormonal coil (brands include Mirena, Levosert, Benilexa, Kyleena and Jaydess) tops our overall satisfaction ratings – with an average 3.6 out of 5.
The hormonal coil lasts 3 to 8 years depending on the brand, is very effective, and women are reporting lots of benefits. Lowdown data shows that it doesn’t seem to negatively impact mood or reduce women’s sex drive as much as other methods like the pill, implant and injection.
47% of women at The Lowdown report that it caused their periods to stop (which many women like) – and it is successfully used by lots of women who suffer from heavy bleeding and conditions like endometriosis.
Lowdown user reviews
“I’ve been using the Mirena for 19 years. It’s brilliant, periods have stopped, there is the occasional spotting every 6-12 months. I don’t have to remember to take it each day. Myself and many of my female family members and friends are on it and all talk positively about it.”
“I have used the coil for best part of 20 years after my now 20 year old son was born. I would highly recommend, after trying the pill before this, hated that!”
“The day I had it fitted I had THE WORST cramps I have ever had but I did also have some post smear investigations done at the same time so they probably didn’t help. I had irregular bleeding for about 6 weeks due to having my implant removed and coming off the pill at the same time as having this fitted (hormones all over the place!) 3 months ish in and it’s the best thing I ever did! So side effects of the coil, no bleeding, no remembering to take anything and covered for years. Bonus I feel so much happier/positive, lost a bit of weigh (I do exercise a lot) and increased sex drive”
“I know some women have amazing experiences with the mirena but I certainly was not one of them which is why I wanted to leave a review of my experiences. The actual insertion was not so bad but I ended up having to go back another day to get it put in knocked out as my cervix wouldn’t open. The first few months I got everything under the sun from constant UTI’s and brain fog, migraines, horrible moodiness, recurring thrush and cysts near my ovaries and irregular periods and pain throughout the whole month.
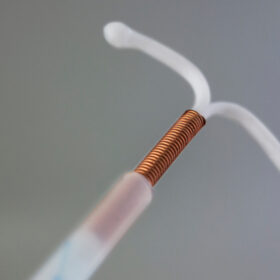
What is the Mirena Coil?
The Mirena Coil is a brand of the hormonal coil. It is a small, T-shaped plastic device that is inserted into the uterus to act as contraception (but can also help manage heavy periods and be sued as part of HRT). It must be inserted by a trained healthcare provider and can last up to 8 years for contraception if under the age of 45 (over the age of 45 you can keep the coil in until you are 55). It can usually be easily removed at any time.
How does the Mirena Coil work?
The Mirena Coil, like other hormonal coils, prevents pregnancy by releasing the hormone progestogen into the womb. This works to thicken the cervical mucus, to prevent the sperm and egg from meeting, and to thin the lining of the womb so a fertilised egg cannot implant. It can also stop ovulation for some people, while for others it will continue as usual.
The progestogen released by the hormonal coil is thought to act “locally”, with lower levels of progestogen in the blood stream than other hormonal contraceptive methods. This means that it may be less likely to cause negative symptoms, for example mood swings. Although we know there are wide differences between users’ experiences, this could help explain why it’s one of the most popular forms of contraception amongst The Lowdown users.
How effective is it?
The hormonal coil is a very effective method of contraception, as it doesn’t rely on the individual remembering to take it or use it.
The hormonal coil is over 99% effective. Less than one user in 100 will get pregnant in one year. To put into context, if 100 sexually active women don’t use any contraception, 80-90 will get pregnant in a year.
How is the hormonal coil inserted?
The hormonal coil needs to be inserted by a trained healthcare provider. Before fitting, they will do a number of tests, including:
- Checking the size and position of your womb
- Checking for any possible STIs and treating with antibiotics if needed
The actual insertion takes between 15-20 minutes. The vagina will be held open with a small speculum, the same way as it is during a smear test, and the coil is inserted through the cervix (the neck of the womb) into the womb. The doctor or nurse will offer a local anaesthetic spray or injection to make the fitting more comfortable.
The hormonal coil has two threads which hang through the opening of the cervix into the vagina. Your doctor or nurse that does the fitting will explain to you how to feel for these threads and check the coil is in place.
If you are worried or cannot feel the threads, you should use additional contraception such as condoms and contact your doctor or nurse. They may suggest a check up and will consider the need for emergency contraception. Otherwise you will only need to go back when the coil needs to be replaced.
How long does it take the hormonal coil to prevent against pregnancy?
The hormonal coil can be fitted at any time during your cycle. If fitted in the first five days of your menstrual cycle you will be immediately protected from pregnancy. If fitted any other time, you will need to use extra protection (i.e condoms) for the first seven days.
If you have a short menstrual cycle, where your period normally comes every 23 days or less, check with your healthcare professional as you might ovulate early in your menstrual cycle.
How is the hormonal coil removed?
The hormonal coil can be removed at any time – but must be done by a doctor or nurse.
The procedure is usually simple and quicker than when inserted. It is removed by gently pulling on the threads, making the T shape fold up so it is easily pulled out of the womb.
If you have the coil removed but you don’t want to get pregnant, use additional contraception, such as condoms, for 7 days before you have it removed. Ideally if you have another form of contraception that you wish to switch to, speak to your doctor beforehand as you may be able to start this before your coil is removed. If you’re having the hormonal coil replaced, your doctor or nurse will normally recommend you still use condoms for 7 days before the removal. This is in case there is a problem with fitting the replacement coil, although this is rare.
Normal fertility should return to your baseline once the coil has been removed.
When should you seek advice from your doctor or nurse after fitting?
Initially afterwards fitting, you may experience light bleeding and period-like cramps which you can take over the counter pain relief for. However if you experience severe or prolonged tummy pain, you feel unwell, especially with a fever, or you feel hot or clammy, you experience heavy bleeding or smelly discharge or you are concerned, please contact your doctor.
Advantages of the hormonal coil
- It is effective for 3 to 8 years (depending on the brand)
- It is one of the most effective forms of contraception available
- It does not interrupt sex
- It is safe to use whilst breastfeeding
- It is not affected by other medicines or illnesses such as vomiting and diarrhoea
- Your periods may be less painful and become lighter, shorter, or stop completely
- It is possible to get pregnant as soon as it is removed
- There’s no evidence that a contraceptive coil will affect your weight or increase the risk of cervical cancer, cancer of the uterus or ovarian cancer
- It is suitable for women who can’t use contraception containing oestrogen.
Side effects of the Mirena coil
- It may cause some irregular bleeding or spotting, which should settle down after the first 3-6 months. Your periods may stop altogether whilst using the hormonal coil, which may not be suitable for some women.
- It can cause temporary side effects such as skin problems, headaches or breast tenderness
- It can cause small fluid-filled cysts on your ovaries which often have no symptoms and disappear without treatment.
Risks of the hormonal coil
- There is a small risk of getting an infection after the coil is inserted, this could lead to a pelvic infection if not treated.
- There is a small risk of the coil becoming pushed out or being displaced. This is more likely just after fitting and within the first 3 months (1 cases in 20). This is why it is important to check you can feel the coil threads in place
- There is a very small risk of damage to the uterus (1-2 cases in 1000).
- If you do become pregnant while you are using the coil (which is very rare) there is a small risk of ectopic pregnancy
- Lastly, there may be an association between current or recent hormonal coil use and breast cancer, however, any potential increased risk appears to be small.
Is it safe to use a menstrual cup with an IUS?
There hasn’t been a large number of research studies looking at coil and menstrual cup use, but some evidence suggests there might be a slightly increased risk of your coil coming out while using a menstrual cup. There doesn’t seem to be any increased risk of infection while using an IUS and menstrual cup.The moon cup manufacturers advise to wait 6 weeks after insertion of an IUS before using a moon cup. It is also advised that the cup be placed with an adequate seal low in the vagina. The seal needs to be broken first before the cup is removed to ensure your IUS is not dislodged. It is important to check your threads after your period, to ensure your IUS is not dislodged. If you have any concerns, speak to your GP or sexual health clinic.
Non contraceptive benefits / uses
- It can make your periods lighter, shorter and less painful or stop them altogether. For women who experience painful or heavy periods, and associated conditions such as iron deficiency anaemia, the benefits can be life-changing.
- It may also be used to treat other conditions that your doctor or nurse may discuss, but these will be on an individual basis.
- The Mirena coil can be used alongside oestrogen therapy as a component of hormone replacement therapy to treat symptoms of the menopause.
Different types of IUS
There are five types of the IUS available in the UK – Mirena, Levosert, Benilexa, Jaydess and Kyleena. However, not all GP surgeries or sexual health clinics will offer all options. This is normally dependent on the training of the practitioner and if the hormonal coil is being used to treat medical conditions, as well as to provide contraception. If the choice is available, this will be discussed with you during the appointment.
Our medical review process
This article has been medically reviewed for factual and up to date information by a Lowdown doctor.