Intrauterine device (IUD) – everything you need to know
What is the IUD?
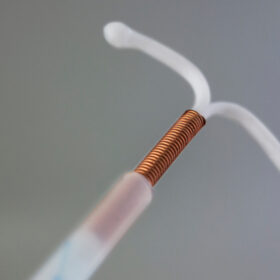
The intrauterine device (IUD), also known as the copper coil is a small T-shaped plastic and copper device that’s placed into your womb (uterus). Most copper coils are made of a T-shaped frame of polyethylene (plastic) and barium sulphate with copper wire wound around the vertical arm. It is a non-hormonal form of contraception. Getting pregnant with the copper IUD is unlikely as it is 99% effective.You can look through the contraception reviews at The Lowdown to see how people like you experienced having the IUD, or you can leave your own to guide others.
How does the IUD work?
It releases copper into your womb which prevents pregnancy by affecting sperm motility, preventing egg fertilisation and possibly preventing implantation. It can protect from pregnancy for 5 or 10 years, depending on the brand, which takes away the stress of having to keep track of what pills you’ve taken or what injections you’ve had.
How do I get started?
To get a coil fitted you will need to go to a GP surgery or sexual health clinic where certain staff are trained to fit them. You can contact your GP and ask if they fit coils, or search for clinics that fit coils here. Your doctor or nurse will do some tests to make sure that you can have the coil – like making sure that you’re not pregnant and checking for infections or STIs.
The coil can be fitted in the first five days or your menstrual cycle (day 1 is the first day of your period), or at any time during your cycle as long as you’re not pregnant or at risk of pregnancy from unprotected sex. Because of the way the copper coil works it can also be used as emergency contraception so this may be an option if you’ve had unprotected sex.It may also be easier to fit the coil at the start of your menstrual cycle during your period (although you may prefer to get it fitted when you’re not on your period).
Your doctor or nurse will use a speculum (like when you have a smear test) to open up your vagina and then insert the coil through the cervix into the womb. This can be uncomfortable. There is an option to have a local anaesthetic to help with the pain and you may be advised to take painkillers, so make sure to discuss this with your doctor or nurse before the procedure.
Once the IUD has been fitted, it is effective straight away. You will be taught how to check the coil is in place by feeling for the threads. GP practices and sexual health clinics may offer you an appointment after 3 to 6 weeks to examine you to check the coil and make sure everything is ticking along smoothly. Be sure to alert your GP if you have any problems after this initial check, or if you want to have the IUD removed.
There is a small risk of an infection following IUD insertion which if left untreated may lead to a pelvic infection. You may have an infection if you:
- Have pain in your lower abdomen
- Have a high temperature
- Have an odour or increased unusual discharge
Side effects of the copper IUD are that it can make your periods heavier, longer and more painful in the first 3-6 months after it is fitted and you may also get spotting or bleeding in-between periods. 61% of Lowdown users claimed it made their periods heavier. Treatment for heavy periods is available from your GP and can include non-hormonal medications such as tranexamic acid or mefenamic acid. Some people claim the copper coil causes weight gain, but there is no evidence to support this and 76% of our users state that their weight had not changed.
How to tell if your IUD is still in place
The IUD has 2 thin threads which hang down slightly from your womb which you should be able to feel at the top of your vagina. Whoever fits your IUD will teach you how to feel for these threads. It’s recommended to check that the IUD is in place a few times in the first month, then at least after each period.
It’s unlikely that your IUD will come out, but it can happen in around 1 in 20 cases, and usually these happen within the first 3 months. If you are unable to feel the threads or think it may have moved, you may not be protected from pregnancy. If this happens use additional contraception, e.g. condoms, until your IUD has been checked by your doctor or nurse. Your partner should not be able to feel your IUD during sex but if they think they can you may want to see your GP or nurse for a check-up. Sometimes the threads can be trimmed and this may be more comfortable.
What about the IUD removal?
Your coil can be removed at any time by a trained doctor or nurse. It’s simpler than having it fitted – they will gently pull on the threads and the T shape folds up and it can be pulled out of the womb.
If you’re not having another coil put in and don’t want to get pregnant, you’ll need to make sure you don’t have sex seven days before you have it removed, or use condoms or another method.
Check out our survey results to see how long it took most women’s cycles to return to their definition of ‘normal’ and read up about other after-effects they’ve experienced.
IUD vs IUS
The IUD (copper coil) and the IUS (hormonal coil) are very similar, however the one significant difference being HOW they prevent pregnancy. The IUD works by realising copper into the body to prevent pregnancy, whereas the IUS releases a hormone called progestogen into the body. The IUD may be favoured by women who want to avoid hormonal contraception. You can use our contraception comparison to further inform yourself.
Pros of the IUD
- Protects from pregnancy for 5 or 10 years
- Once fitted, it is effective straight away
- Most women are able to use it
- There are no hormonal side effects
- It does not interrupt sex
- Safe to use whilst breast feeding
- Not affected by other medicines
Cons of the IUD
- Small risk of infection after it’s been fitted. This may occur when harmless bacteria normally found in vagina are pushed inside the womb. Contact your doctor if you are worried you have an infection or experience unusual discharge, abdominal pain, or you develop a high temperature or chills
- Around 1 in 20 coils can fall out or be pushed out by the womb; this is most common in the first 3 months after getting it fitted, or during a period. If this happens, you are not protected from pregnancy and will need to use another form of contraception
- If the coil doesn’t work and you get pregnant (which is very unlikely as the coil is more than 99% effective), there’s also a small increased risk of ectopic pregnancy – when the fertilised egg implants outside the womb, normally in the fallopian tubes. However, the overall risk of ectopic pregnancy is less in women using a coil than in women using no contraception at all.
- Very occasionally the threads get lost. This happens to about 1 in 100 women, and is more commonly caused by the threads being pulled up inside into the cervix. They may notice this when you go to have the coil removed, and sometimes the threads can reappear naturally.
- Even more occasionally (1 in 1000 chance) the coil may damage the wall of the womb. This is called ‘perforation’ and if this happens you won’t be protected against pregnancy and occasionally the coil will need to be removed by surgery.
Who should use the IUD?
- want a contraception that is long lasting
- want a non-hormonal form of contraception
- are breast feeding or taking medicines that may affects some forms of hormonal contraception
- think they might be pregnant
- have an untreated STI or pelvic infection
- have anatomical problems with their womb or cervix
- have unexplained bleeding between periods or after sex
- have a condition called Wilson’s disease which causes higher levels of copper in the blood stream
Where can I get the IUD?
In the UK, you are able to get the IUD for free, even if you’re under 16. You can get it from most contraception clinics, some GPs surgeries and some young people’s services.
Our medical review process
This article has been medically reviewed for factual and up to date information by a Lowdown doctor.






