Does birth control affect your sex drive?

This guide has been peer reviewed by the medical team at The Lowdown and the CoSRH and is regularly reviewed as per both clinical content policies
In this article
What's the lowdown?
Sex drive is complex, and influenced by many different cultural, social, psychological and biological factors
There is no concrete evidence that hormonal contraception affects sex drive, however other side effects of hormonal contraception, such as vaginal dryness, may indirectly affect libido
If you are prone to experiencing low mood when taking hormonal contraception, you may be more likely to experience a reduced libido
Aroused, libidinous, turned on or just plain horny: sex drive has a million weird and wonderful names, and it’s time we started talking about it.
If you’ve found your way here, you’ve probably got some questions about libido. Maybe you’ve noticed a change in your sex drive since you started a new contraceptive method, or are doing your research before you talk through your options with your GP. Whatever your queries about contraception and sexual drive, we’ve got you covered. But first, let’s have a look at what sexual drive actually is.
What is libido?
Your libido is your sexual appetite, so in reality how frequently you want sex, and how strong your interest in it is. Libido can be influenced by a number of factors, including hormones, lifestyle and overall physical health.
When we talk about ‘losing our sex drive’ or ‘having a low libido’, though, we don’t always mean that it is only our desire for sex that has changed. There are actually a few different factors that can contribute to our enjoyment of sex, and it’s important that we understand what those are before we make decisions about our contraception.
What causes low libido?
Sex drive is a mammoth subject, especially when it comes to women. Like most things to do with our health, it’s woefully under-researched and women can feel ashamed to speak about libido and the way it impacts their lives. It’s also really difficult to specify precisely what might be causing changes to libido, because there are so many societal, cultural, psychological and physiological factors that can play a role.
One study¹ has explored these factors. In 2017, researchers from Kentucky asked 31 women to answer questions about their experiences of sexual desire. They found that cultural gender expectations – what is ‘expected’ of women – can impact sex drive and libido. Particularly within the LGBTQ+ community, a lack of visible or safe spaces can have an influence, and religion, taboo and changing cultural times were also picked up as themes within the research, demonstrating how multifaceted and complex sexual drive really is. These factors don’t just influence how interested we are in sex, either. They can affect your arousal (the physical and emotional effects you feel when engaging in or thinking about sex, like lubrication), your satisfaction (whether or not you orgasm, or are satisfied with how the sex made you feel) and can even cause us to experience pain during intercourse.
Why is this important?
Everyone is different, and so what they hope or wish to experience during sex is different, too. For one person, physical intimacy might be an indication of a satisfying sexual experience, while for another, orgasm might be really important. For some, simply removing the potential for an unexpected pregnancy greatly improves their enjoyment of sex.
This is completely subjective, so it’s important that you know what a positive sexual experience means to you. That way, when you’re making choices about your contraception, you can prioritise accordingly.
Now, let’s get into the big question…
Does birth control affect your libido?
A lot of what we hear about sex drive and contraception is anecdotal, such as stories from friends, and while this is still really important, it doesn’t give us any real scientific answers as to whether specific contraception can cause changes to libido.
Like we said, there’s a lack of research when it comes to this question, and the evidence that is out there isn’t always consistent.
That being said, let’s go through what science can tell us.
What does science tell us about contraceptives and libido?
A review² looking at all of the evidence surrounding combined contraception and libido until 2012 found that a small number of women experienced an increase or decrease in libido, while the majority of participants across studies experienced no changes to their sexual desire at all.
Another review³ found there to be no consistent pattern among participants – as in the above study, some experienced reduced libido, others experienced heightened libido, and most experienced no change whatsoever. The researchers here suggest that any changes might be due to a complex interaction of psychological, social and biological effects, like we mentioned earlier, which are really difficult to tease apart.
Combined hormonal contraception: does the pill reduce libido?
Combined hormonal contraception is any form of contraception that contains both oestrogen and progestogen. This includes some pills, the patch and the vaginal ring.
Oestrogen may play a role in changes to sexual drive in some women. Interestingly, combined hormonal contraceptives containing lower levels of oestrogen seem to have a greater impact on sexual drive than those containing higher levels.⁴ ⁵ Again, though, this appears to affect only a small number of women.
Combined hormonal contraception has also been found to lower the levels of testosterone in the body.⁶ There is some evidence that testosterone can influence libido in women.⁷ In one study,⁸ which looked at women aged 18-35, testosterone was found to be lowered following combined hormonal contraception, but this had no significant impact on sexual drive. It is thought that the effect of testosterone on libido could be affected by the sensitivity of an individual’s androgen receptors (the receptors in the brain that bind testosterone). Essentially, whether or not your libido is affected by changing levels of testosterone could just be down to your unique biology. Helpful, we know.
Combined pill regimens
Research has found that certain pill regimens (the way you take your pill) may have an impact on sexual function. There is evidence⁶ that the more ‘hormonal days’ you have – the days on which you take a pill – the more sexual function may be improved. One research study⁹ found that those taking a new, low-dose combined contraceptive pill, with a reduced hormone-free interval (shorter pill free week, had generally improved sexuality over time. The same researchers¹⁰ also found that a continuous contraception regimen could worsen the quality of a woman’s sexual life before causing an improvement. More research is definitely needed here.
Progestogen-only contraception
Progestogen-only contraception is hormonal contraception that only contains the hormone progestogen (we really over-explained that one, didn’t we?). It does not contain oestrogen. The mini pill, the injection, the hormonal coil and the implant are all types of progestogen-only contraception.
The effects of progestogen-only contraception on libido aren’t well studied, but the current evidence suggests that it does not have a negative impact on sexual drive.¹¹ No research has found a significant link between progestogen-only contraception and libido changes.
Hormonal contraception in general
While the jury seems to be out on whether hormonal contraception directly affects libido, there is the possibility that it could be indirectly causing a drop (or rise!) in your sex drive
Can hormonal birth control indirectly affect libido?
Hormonal contraception does come with some side effects that have a bit more research evidence, and there’s a chance that these might be impacting your libido, arousal and sexual satisfaction.
Some people find that the hormones in their contraception cause vaginal dryness, which might not affect your interest in sex, but may impact how much you enjoy it. All hormonal contraceptives also come with a warning that they may cause mood changes, too, so if you’re experiencing low mood, this could be an indirect cause of a reduction in your libido.
Additionally, one study has found that those who have negative mood side effects from their hormonal contraception are more likely to also experience sexual side effects,¹² so that’s something to bear in mind.
On the other hand, there are obviously some positive consequences of taking hormonal contraception – we do it for a reason, right? It reduces your risk of pregnancy, which can mean you feel less worried about protecting yourself during sex and can just go with the flow (although it doesn’t protect against STIs, which only condoms do). If taking the pill every day is something you struggle with, a more long-term form of contraception, such as the hormonal coil, implant or injection, may help to reduce any worry that might be impacting your interest in or enjoyment of sex.
Hormonal contraception can also reduce the length, pain or heaviness of your periods, which some people find improves their interest in sex. Of course, there are some people who find that their periods are longer or heavier on hormonal contraception, so this is something that could have the opposite effect, too.
If you’re finding that your sex drive has been affected since you began taking hormonal contraception, it might be worth thinking about other side effects you might be experiencing that could be having an impact and what else is going on in your life. That way, you can talk to your GP about changing over to something that might have less of a risk of a particular side effect.
You could also consider non-hormonal contraception such as the copper coil. These methods of contraception are unlikely to directly impact your sex drive.
What are The Lowdown users saying?
Our users tell a different story to the research. As of December 2022, this is what our current review data tells us
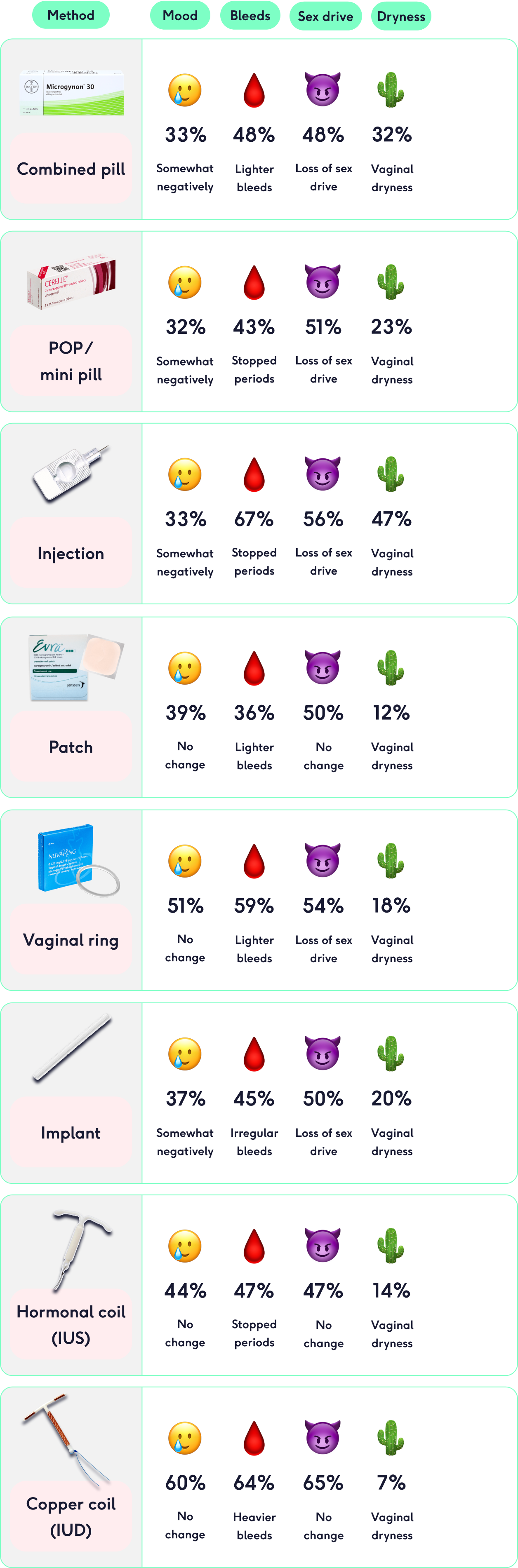
51% of progestogen-only pill users said that they had experienced a reduction in libido. 9% reported an increase in sex drive, and 30% said they had experienced no change.
Combined pill users were only slightly behind this figure, with 48% of them telling us that the pill had caused caused them to experience a loss in sex drive. While 7% saw an increase, and 30% saw no change.
50% of implant users also reported a reduction in their sex drive, with 6% seeing an increase and 28% experiencing no change. The highest percentages of people who saw a reduction in their libido were vaginal ring users, at 54%, and injection users at 56%.
There are other hormonal contraceptives that our users felt had less of a negative impact on their sex drive. Only 29% of hormonal coil users saw a drop in their sex drive, and patch users just 19%.
These figures are much higher than the current scientific evidence would suggest. It’s worth mentioning that people are more likely to leave a review when they have had a negative experience, but this is still really important; the effects of hormonal contraception on libido are under-researched and we need to hear these stories. That being said, it’s less common for positive outcomes to be reported, so we definitely need more research in this area.
It’s also really important to remember that, as we said before, sexuality is really complicated. What impacts the libido of one person might have no effect on another, and when it comes to contraception, there is no one-size-fits-all answer.
What should I do if I feel my contraception is affecting my sex drive?
If you feel as though your contraception is having a negative impact on your sex drive, you certainly aren’t alone, and you have lots of options available to you.
As a first port of call, it’s always good to speak to your GP. They will be able to discuss whether there might be other reasons for any issues you might be facing, and will be able to suggest alternative methods of contraception if they feel it might help.
We’d also recommend having a look through our contraception review, to see whether this is something that others have experienced, and whether anyone with similar issues had better results with a different type of contraception.
Sex drive in women is a complex and under-researched area, but one thing is certain: if you feel your contraception is having a negative impact, you don’t have to just put up with it.
This blog can help you learn more about various contraception options, but it does not give medical advice. You should always speak to a nurse or doctor when making choices about contraception and before starting a new method.
Our medical review process
This article has been medically reviewed for factual and up to date information by a Lowdown doctor.